Do You Need a Measles Booster?
A 43-year-old Israeli flight attendant recently contracted measles, leading to encephalitis (brain inflammation) and a coma. While a measles outbreak is currently affecting nearly half of U.S. states, most people being infected haven’t been vaccinated. What’s different about the Israeli flight attendant? She had been inoculated against measles.
How did she get the measles? She only received one of the two recommended inoculations, leaving her susceptible to the virus.
Who is Most Affected by Measles?
Measles is very serious, highly contagious, airborne virus that can lead to a wide range of complications such as pneumonia, encephalitis, ear infections, hearing loss and even death if not treated. Although measles is often associated with babies and young children, you can contract it any age.
Vaccinations helped public health officials gain control over the virus. In 2000, the Centers for Disease Control and Prevention (CDC) declared measles eradicated from the United States. The last case of measles in the Americas during that period was in late 2002, so declarations from other North, Central and South American nations shortly followed.
Measles reemerged around 2010. Each year since 2010, the CDC has reported a measles outbreak—the worst year so far has been 2019. And the year isn’t half over yet.
How is Measles Making a Comeback?
Children going unvaccinated has had a huge effect. The 2017 National Immunization Survey-Child reported a 0.3 percent rise from 2001 in the number of children under 24 months who have not been vaccinated. The survey also showed an annual rise over the last three years of vaccine exemption rates among infant and school-aged children.
The second problem is that the measles vaccine is only 90 percent effective. In 1989, public health officials began recommending an MMR (measles) booster to raise the efficacy to 97 percent.
Measles is highly contagious. When an unvaccinated child, for example, travels to an area where the virus is active – to India or Eastern Europe or the Philippines — they can become exposed. They can then spread measles to other unvaccinated children, infants too young to be vaccinated and adults who may have missed their MMR booster or who may never have been vaccinated themselves.
“An infected person can spread the virus to others for about eight days before they even realize they may have it, making public places -- schools, churches, daycare centers, pediatrician offices, restaurants, supermarkets, airports, airplanes – unbeknownst breeding grounds for measles,” says Bernard Kaminetsky, MD, medical director, MDVIP. “And children under five and adults over 30 are at the biggest risk of developing measles-related complications.”
How to Lower Your Risk of Contracting Measles
Here are a few steps you can take to lower your risk of contracting measles:
- Make sure you and your family are up-to-date on MMR vaccines and boosters.
- Understand the signs and symptoms of measles, including fever, dry cough, runny nose, sore throat, red eyes, white spots lining the inside of the mouth and cheeks, and a large, flat, blotchy rash.
- If you develop symptoms, visit a healthcare provider, avoid work/school and social obligations for at least four days after the onset of the rash and isolate yourself from high-risk people such as young children, pregnant women and anyone who hasn’t been vaccinated.
- Visit the CDC's website to learn more about measles.
Who Should Consider Getting a Measles Booster?
“If you were born before 1989 — but after 1956 — discuss getting an MMR booster with your primary care physician,” Kaminetsky says. People born before 1957 are generally considered immune due to exposure to the live virus.
If you don’t have a primary care physician, consider partnering with an MDVIP-affiliated physician. They have time to really work with you to develop a wellness plan that can help you focus on preventing or controlling heart disease. Find a physician near you and begin your partnership in health »
Adult Vaccination Schedule
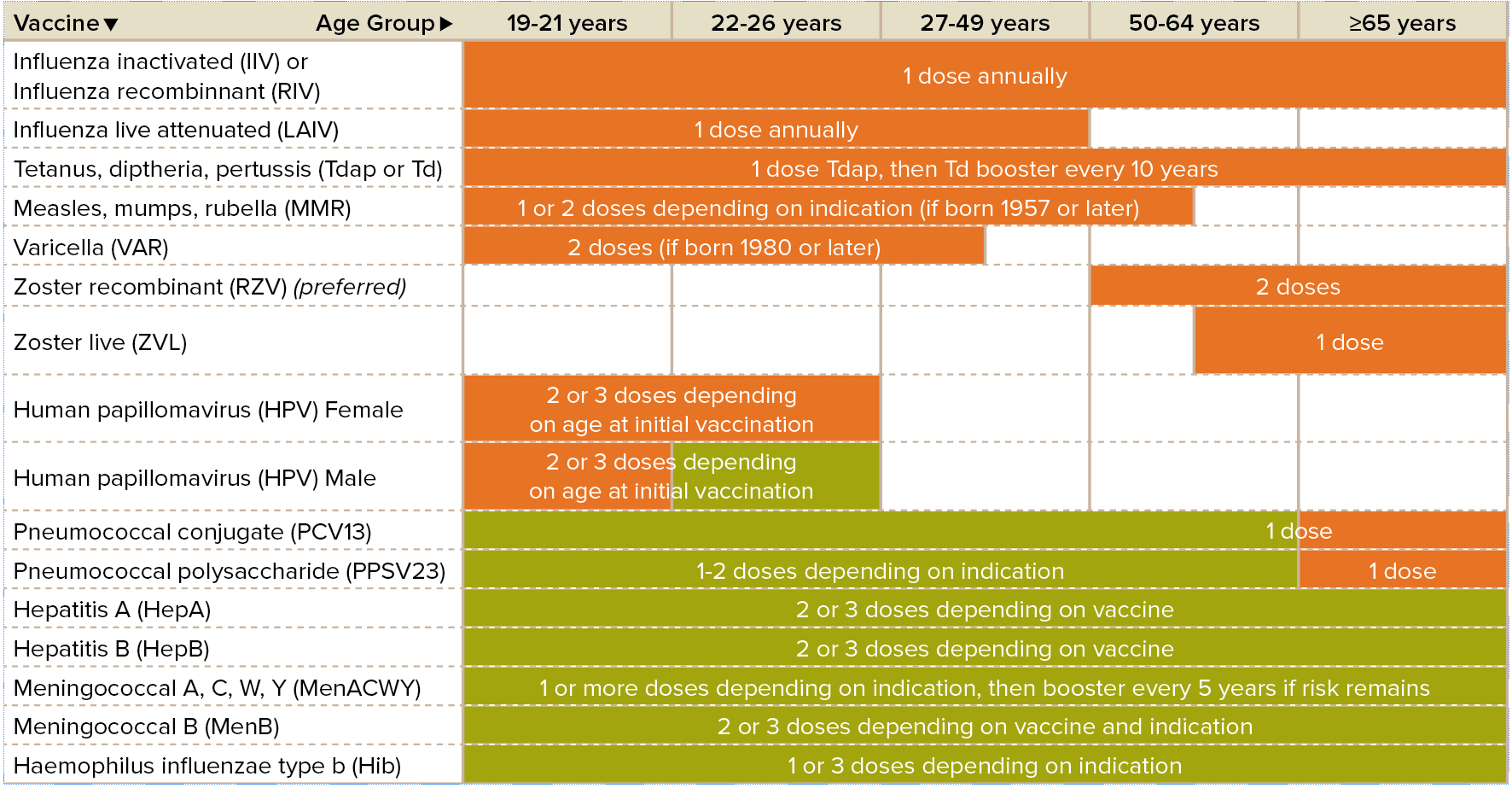
Orange is recommended vaccination for adults who meet the age requirement, lack documentation of vaccination or lack evidence of past infection.
Green is recommended vaccination for adults with an additional risk factor or another indication.
*Recommended Adult Immunization Schedule by Age Group | United States 2019
