4 Tips to Help Prevent Estrogen Dominance, A Risk for Breast Cancer in Women and Men
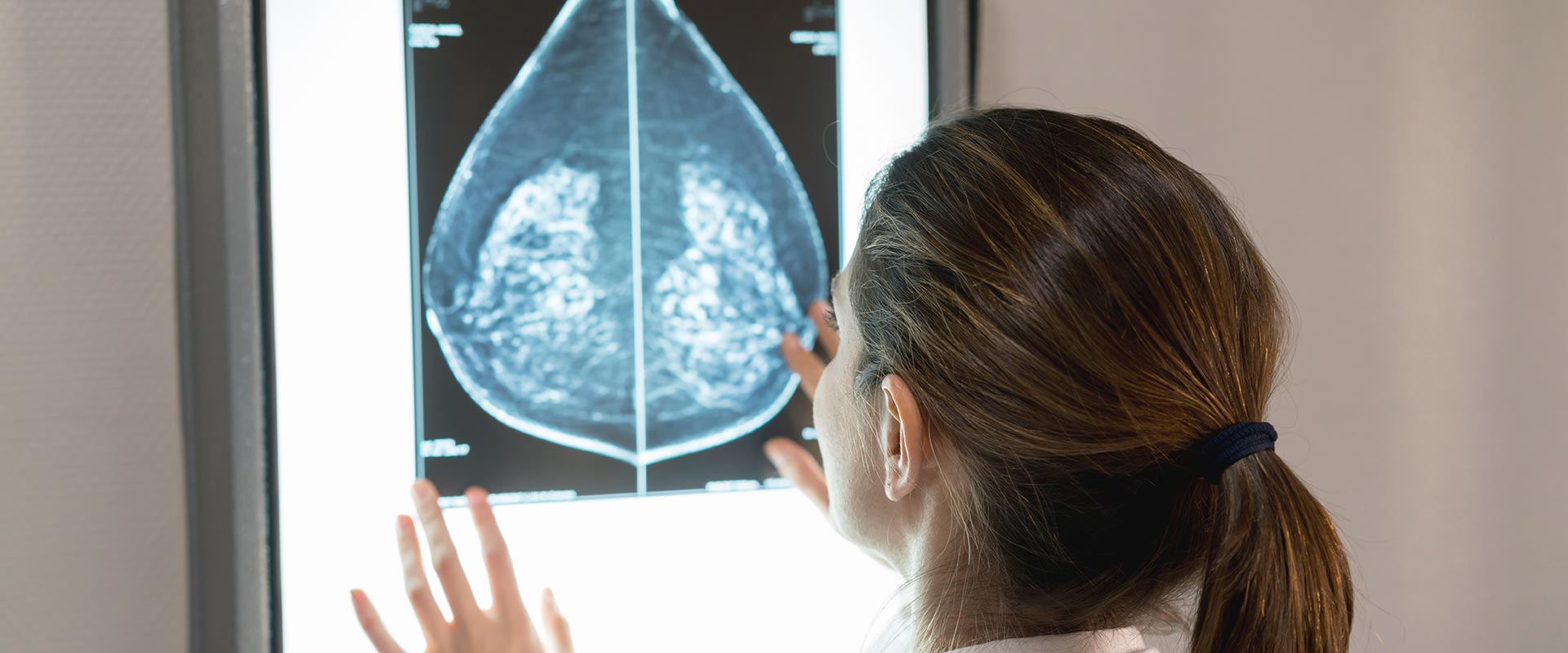
Low estrogen levels in women can cause weight gain, mood swings and headaches. It also raises the risk for cardiovascular disease, osteoporosis and dementia. And in men it may raise body fat, lower sex drive and contribute to erectile dysfunction.
Seems awful. But there is one bright spot – lower levels of estrogen also lower your risk for breast cancer as well as other estrogenic cancers such as ovarian, uterine, thyroid and prostate. A pooled analysis involving nine studies suggested that having high levels of the estrogen estradiol doubles your risk for breast cancer, according to the Susan G. Komen Foundation.
“There are different types of estrogen,” says Dr. Andrea Klemes, endocrinologist and chief medical officer, MDVIP. “Low levels of one type can lead to a host of health issues, while high levels of another type raise the risk for cancer.”
Estrogen is a group of female hormones comprising estrone, estradiol, estriol:
- Estradiol is the estrogen that keeps us looking and feeling young. It’s produced by the ovaries in women and derived from testosterone in men. It promotes our sex drive and helps protect us from cardiovascular disease, osteoporosis and cancer. Levels beginning waning in your 30s. It’s pretty much depleted in women by menopause, but it varies in men.
- Estriol and estetrol are the pregnancy estrogens. Your body releases estriol during pregnancy to provide nourishment to the placenta. Recent studies credit it with anti-inflammatory properties and link it to gut health. The fetus’ liver produces estetrol, though its function is unclear. After giving birth, levels of both hormones become undetectable.
- Estrone is known as the menopause estrogen. It’s secreted by ovaries, converted by testosterone or produced by fat tissue. This is why some experts consider being overweight a risk for certain cancers. Although it helps protect the heart and brain in women and men, it can cause some weight gain, raise the risk for estrogenic cancers and has been linked to type 2 diabetes and atherosclerosis in men.
Genetics are involved in breast cancer but not as much as you might think. Less than 15 percent of breast cancer cases have familial ties, according to BreastCancer.org. Hormones play a role in at least some types of breast cancer.
Breast cancer has lots of potential causes, according to National Institute of Environmental Health Sciences-funded research. Causes include smoking, excessive alcohol consumption, exposure to ionizing radiation and being overweight, particularly after menopause. Taking combination hormonal therapy products (estrogen and progesterone together) and using of diethylstilbestrol (or DES) – a medication used years ago to prevent miscarriages and premature deliveries are also considered potential causes.
However, estrogen also plays a critical role in the development of breast cancer, according to a study published in Cancer Letters. Researchers found that cells involved in estrogen-receptor (ER) positive breast cancer cells – one of the most common forms of breast cancer -- need estrogen grow.
Every month a woman’s menstrual cycle stimulates breast tissue with estrogen that can attach to hormone receptors of breast cancer cells, so the fewer menstrual cycles you have, the lower your risk for ER positive breast cancer. That’s why three risk factors for breast cancer include: beginning menstruation before age 12, starting menopause after age 55 and never getting pregnant. And since women have more exposure to estrogen, particularly estrone, their breast cancer rates are higher than men’s.
Sometimes the body produces an imbalance of hormones -- in women it’s a high estrogen to progesterone ratio and in men it’s a high estrogen to testosterone ratio. There are three usual causes for this: Hormone replacement therapy (HRT), genetic issues or lifestyle issues. This is called estrogen dominance.
HRT is often prescribed for severe perimenopausal or postmenopausal symptoms, surgically-induced menopause It’s typically intended for short-term use. Although there are different types, some experts consider long-term HRT use to be risky.
Genetic issues also occasionally interfere with the body’s ability to process and get rid of excess estrogen. Lifestyle issues like diets high in processed foods, chronic stress, poor liver function, inadequate sleep and substance use also contribute.
“Estrogen is metabolized in the liver. This means if you’re liver isn’t healthy, it can affect how estrogen is metabolized,” Klemes said. This can lead to elevated levels of estrogen in the body.
It’s not always easy recognizing the symptoms of estrogen dominance, especially in postmenopausal women, as typical symptoms include irritability, insomnia, headaches, depression, weight gain (particularly through the hips), uterine fibroids, ovarian cysts, memory issues, low sex drive, premenstrual syndrome and fatigue. In men, it’s usually enlarged breasts, sexual dysfunction and infertility. It’s often related to or mistaken for low testosterone.
Estrogen dominance and buildup of bad estrogen metabolites may not be completely preventable, but you can take some steps to help control both issues, such as:
- Exercise: helps lower estrogen levels and control body fat, which releases estrogen. Talk to your doctor about starting an exercise program.
- Choose organic, whole, plant-based foods: because they aren’t sprayed with pesticides, herbicides or fungicides that may disrupt your hormones. They also don’t have the hormones, whether naturally occurring or injected into the cattle.
- Avoid plastic containers and bottles: they contain xenoestrogens – natural or synthetic compounds that imitate estrogen. They’re found in many plastics. When possible, store your foods and beverages in glass. Just as a heads up: Xenoestrogens are commonly found in many cosmetics, hair, skin care and hygiene products. There isn’t any federal regulation on these items and they’re nearly impossible to cut out or your lifestyle.
- Manage stress: when stressed, your body uses progesterone (the other female hormone) to create cortisol, which helps your body handle the stressful situation, but it leaves an excess of estrogen in its wake.
Managing your hormones is not easy. But your primary care physician may be able to help. Need a primary care physician? Check out MDVIP, a nationwide network of primary care doctors who focus on personalized medicine and prevention and have the time to develop close, doctor-patient relationships. Find one near you and begin your partnership in health »
This content was last reviewed and updated during February 2021.
